“I remember saying to the doctor, ‘Is she at that point?’” Judi Stout recalls of one of two pivotal moments of her daughter’s experience in the Intensive Care Unit (ICU) at Hillcrest South. The second occurred when the off-duty nurse manager woke in the middle of the night concerned about Candace’s scheduled x-ray and told the nursing staff to wait until the next day.
Candace Stout, 27, went into respiratory distress February 17, 2014 and was transferred from W.W. Hastings Hospital in Tahlequah, OK to Hillcrest South. Candace’s parents Judi and Jack were relieved their daughter was coming to Tulsa. “As fate would have it, Hillcrest South was the only hospital in Tulsa with an ICU bed,” Judi says.
Candace was born with Down’s syndrome. She suffered from asthma and had been diagnosed with Acute Respiratory Distress Syndrome (ARDS) in 2013. Respiratory problems in children with Down’s syndrome are one of the leading causes for hospitalization and often result in admission to the ICU. Judi knew her daughter’s situation was severe when they arrived at Hillcrest South. “She was placed on a Rotoprone bed for five days as a last resort,” shares Judi. She says one of Candace’s doctors asked if a DNR order was in place. That is when she replied, “’Is she at that point?’”
Judi says the support of her husband constantly by their side, a strong network of friends and family and her faith helped her stay strong, believing God would heal Candace through her doctors and medicine. To monitor Candace’s status, a chest x-ray was given every morning at 3 a.m., but it was difficult for Candace to maintain her oxygen levels after the process. “We started to notice she wasn’t tolerating being turned,” adds Judi. “I went to the chapel and started praying for her.”
That same night, Judi says, the charge nurse overseeing Candace’s care during the day woke from sleep at home. “He was worried about her,” shared Judi. “He texted the charge nurse to not do the chest x-ray that night.”
The next day, nurses positioned Candace differently during the x-ray and manually bagged her oxygen during the process. It was the change she needed to make a turn in her progress. Medication began to start working to clear her lungs. Soon she was strong enough for physical therapy. “Every step of the way was so exciting,” shares Judi of her daughter’s healing.
After five weeks, Candace was strong enough to be transferred to a long-term acute care center in her hometown, Muskogee. She returned home following another three-and-a-half weeks of rehabilitation. Candace and her mother have returned twice to visit her doctors, nurses and staff. “Everyone was wonderful,” Judi adds. “We really appreciate everything. We were treated like family.”
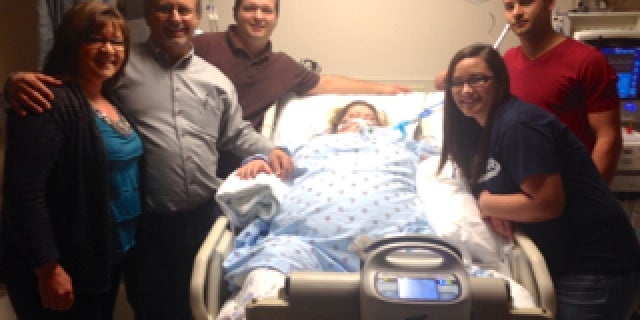
Judi shared her appreciation for the care her daughter received by putting together a musical montage of photos from Candace’s stay in the ICU. She calls it “the thought of our hearts” and gave a copy to the staff. Pictures like this one capture memories of triumph and the team who helped make it possible.
